Intertrochanteric Hip Fracture in a 4-year child: A Case Report
R. Spagnolo1*, F. Pace2, D. Porreca3
1Department of Orthopaedic Surgery, Asst Hospital Treviglio, Bergamo, Italy
2First Orthopaedic Clinic-Hospital Gaetano Pini, University of Milan, Italy
3Physiotherapist ASST Bergamo, Ovest-Hospital Treviglio Caravaggio, Italy
Abstract
Hip fractures are rare in children and are less than 1% of all pediatric fractures and less than 1% of all cases of hip fracture. The literature agrees that early treatment, whether surgical or conservative, reduces the risk of complications. The clinical case we present concerns a pertrochanteric fracture with displacement of the greater trochanter in a 4-year-old child. The fracture was a type 4 according to Delbet classification. Clinical evaluation was carried out using the Ratliff scheme. Clinical criteria include pain, movement, activity and X-ray evaluation of the fracture both from the point of view of the formation of the bone callus, and the alteration of the diaphyseal cervical angle (DCA). It was surgically treated with three cannulated screws and a hip spica plaster cast immobilization with a Kirschner wire to avoid secondary displacement. The cast was maintained during the 6 weeks healing period of the fracture. After plaster cast removal, the child begins physiotherapy with an experienced physio in pediatric trauma. The child healed without complications.
Introduction
Hip fractures are rare in children and less than 1% of all pediatric fractures and less than 1% of all cases of hip fractures1. In contrast to adults, hip fractures in pediatrics and adolescents are usually the result of high-energy trauma. The causes are falls during recreational activity (swings, slides in younger children), road accidents with bikes, motorcycles and finally, violence on children. According to fracture pattern, complications of hip fractures can cause osteonecrosis of the femoral head, early closure of the physis, varus or valgum deformity. Literature agrees that early treatment, whether surgical or conservative, reduces the risk of complications2. The clinical case we present concerns a pertrochanteric fracture with a rare dislocation of the greater trochanter in a 4-year-old child.
Materials and Methods
The clinical case we present concerns a pertrochanteric fracture with displacement of the greater trochanter in a 4-year-old child. Clinical and X-ray examinations were assessed using the scheme proposed by Ratliff3. Clinical criteria include pain, movement, activity and X-ray evaluation of the fracture both from the point of view of the formation of the bone callus, and the alteration of the diaphyseal cervical angle (DCA). DCA less than 120° means coxa vara, a CDA more than 150° means coxa valga. If more than 50% of the growth plate is closed, it is defined as an early closure. The shortening or lengthening of the limb evaluated both clinically and radiologically, is considered significant if it is more than 2 centimeters. Fracture reduction was defined as anatomical or acceptable if the fracture line was less than 2 mm and the DCA is less than 5 mm, and not anatomical if they exceeded these parameters.
Clinical Case Description
A four years old child, with no medical history, presented in emergency room with a closed trauma of the right hip, and excoriation of the left forearm and swelling of the right ankle. The girl had fallen from the swing; general examination revealed no other significant injury and no neurological deficits were present. Plain radiographs of the pelvis showed the fracture of the right hip with an important displacement of the proximal femur and the greater trochanter, classified as type 4 according to Delbet (Figure 1). The X-ray investigation was completed with X-rays above and below the fracture to exclude other fractures. The patient was operated after 4 hours from entering the hospital under general anesthesia. To reduce the fracture, we placed a supracondylar 2 mm threaded Kirschner (K.) wire. She was then transported to the operating theatre on a surgical table adapted to the size of the child. Traction was facilitated by applying a bracket to the K. wire to reduce the fracture. The traction has two advantages: to control the length and to avoid rotational defects. After a gentle continuous traction, we obtained a good reduction when checked with intra-op fluoroscopy. The stabilization was achieved by placing percutaneously three 4 mm titanium cannulated screws. The first screw was positioned in the lower-central quadrant of the femoral neck, the second screw anterior, and the third posterior (Figure 2). In the beginning, we unsuccessfully tried with external maneuvers to reduce the condroepiphysary detachment of the greater trochanter, exerting a rear-to-front thrust after the stabilization of the fracture; with the use of a 3mm percutaneous K. wire we reduced the trochanter. Always under general anesthesia, we packed a hip spica cast with a threaded Kirschner wire at the knee level incorporated in the plaster cast, to avoid a possible shortening of the leg, given the type of fracture and the type of fixation. The only screw that guaranteed us good stability was the first one, while the other two were too close to the trochanter fracture. The cast was maintained during the 6 weeks healing period of the fracture. After plaster cast removal, the child begins physiotherapy with an experienced physio in pediatric trauma. She walked independently after 4 months, painless and with a complete range of motion. No angular deformity or shortening of the right lower limb was noted. Three years after the trauma, clinical evolution was normal (Figure 3) and the X-ray of the spine and lower limbs in orthostasis showed proper growth of the femur and a good diaphyseal cervical angle without dysmetria, and a slight scoliotic attitude was evident (Figure 4). Seven years after trauma, the scoliotic attitude has also regressed with targeted exercises.
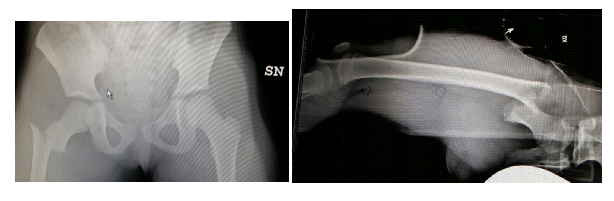
Figure 1: Delbet Tipo IV, 4 years old female with dislocation greater trochanter
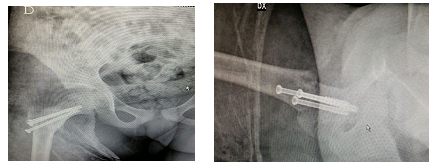
Figure 2: After operation : reduction fracture and greater trochanter
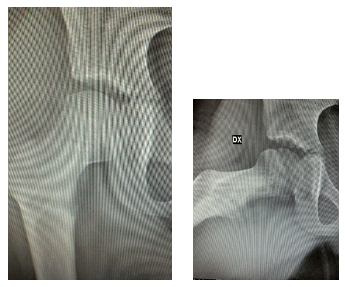
Figure 3: Three Years afer trauma
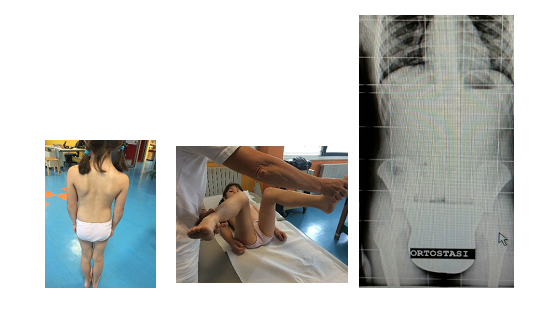
Figure 4: Clinical and radiographic control after four years
Discussion
Treatment of fractures in childhood has seen a significant evolution in recent years. Although indications of surgical treatments have become more frequent than in the past, given technological developments and increased functional demands. Conservative treatment and, in particular, plaster immobilization is still the most frequently applied treatment for fractures in childhood. Reducing patient mobility for more or less prolonged periods is certainly one of the major disadvantages of conservative treatment, as it produces stiffness and muscle hypotrophy. In young people, the rigidity after immobilization usually does not remain more than two weeks after removing the plaster cast, provided that the fracture heals with a formation of bone callus sufficient to ensure early mobilization4. Prolonged immobilization could develop thromboembolism complications; in pediatric age, the risk is frankly reduced compared to adults, so much that in patients under the age of 15 and under 50 kg, in the absence of specific risk factors, antithromboembolic prophylaxis is not always provided4. Some studies have shown that the incidence of complications after femoral neck fractures can be as high as 60%5,6. Delbet's type 4 fracture carries a lower risk of post-traumatic complications. The most frequent complication is secondary displacement after surgery due to insufficient reduction or secondary mobilization in a plaster cast7,8. The incidence of coxa vara ranges from 20% to 30%, which has now decreased due to the increase in surgical treatment2,9,10,11. The case we have proposed gives some reflections about the treatment of these fractures in children under the age of four. Surgical treatment should be carried out within 6 hours from hospital access. Osteosynthesis, when it is compatible with age, should be the primary treatment. The choice of the cannulated screws or dedicated plates are the most used techniques. The experience of the surgeon is important in treating these fractures. If you choose a stabilization that you consider unstable, it is advisable to make a post-operative hip spica plaster cast. As in the case described, the plaster cast must incorporate the supracondylar Kirschner wire, which has an anti-glide effect and therefore can avoid secondary displacement. The cause of secondary displacement in children treated with plaster cast reported in literature is unclear; we have hypothesized that perhaps in many cases, the supracondylar threaded Kirschner (K.) wire was not applied at the knee.
Conclusions
Treatment of fractures of the proximal femur remains controversial. Studies and publications have reported that early reduction and stabilization are the gold standards in the treatment of fractures in pediatric age. In the above case, positioning of the K. wire before surgery helped us a lot during the procedure. Due to the unstable nature of this fracture, hip spica plaster cast with supracondylar threaded K. wire helped to maintain reduction. In conclusion, if in children it is not possible to use the adequate implant, it is advisable to position and maintain the threaded K. wire combined with plaster cast immobilization.
Funding
This study has no sponsorship support.
Conflict of Interest
The authors have no conflicts of interest to declare.
References
- McCarthy J, Noonan K. Fractures and traumatic dislocations of the hip in children. In: Beaty JH, Kasser JR, editors. Rockwood and Wilkins’ Fractures in Children. 7th ed. Philadelphia: Lippincott Williams & Wilkins. 2010; 769-796.
- Dhar SA, Ali MF, Dar TA, et al. Delayed fixation of the transcervical fracture of the neck of the femur in the pediatric population: results and complications. J Child Orthop. 2009; 3(6): 473-477.
- Ratliff AH. Fractures of the neck of the femur in children. J Bone Joint Surg [Br]. 1962; 44: 528-42.
- Madhuri V, Dutt V, Gahukamble AD, et al. Interventions for treating femoral shaft fractures in children and adolescents. Cochrane Database Syst Rev. 2014; 7: CD009076.
- Jackson PC, Morgan JM. Perioperative thromboprophylaxis in children: development of a guideline for management. Paediatr Anaesth. 2008; 18(6): 478–487.
- Bagatur AE, Zorer G. Complications associated with surgically treated hip fractures in children. J Pediatr Orthop B. 2002; 11: 219-28.
- Togrul E, Bayram H, Gulsen M, et al. Fractures of the femoral neck in children: long-term followup in 62 hip fractures. Injury. 2005; 36: 123-30.
- Forlin E, Guille JT, Kumar SJ, et al. Complications associated with fracture of the neck of the femur in children. J Pediatr Orthop. 1992; 12: 503-9.
- Flynn JM, Wong KL, Yeh GL, et al. Displaced fractures of the hip in children. Management by early operation and immobilisation in a hip spica cast. J Bone Joint Surg [Br]. 2002; 84: 108-12.
- Togrul E, Bayram H, Gulsen M, et al. Fractures of the femoral neck in children: long-term follow-up in 62 hip fractures. Injury. 2005; 36: 123-30.
- Bombaci H, Centel T,Babay A, et al. Evaluation of complications of femoral neck fractures in children operated on at least 24 hours after initial trauma. Acta Orthop Traumatol Turc. 2006; 40(1): 6-14.
