Five Key Points on Meniscal Allograft Transplantation
Eric D Haunschild, Ron Gilat, Michael C Fu, Brian J Cole*
Midwest Orthopaedics at Rush, Chicago IL, USA
Abstract
Meniscus injuries are a common presentation to orthopedic clinics, with hundreds of thousands of meniscectomies and meniscus repairs being performed every year1. As the consequence of osteoarthritis progression has been found to be associated with functional meniscal deficiency, a significant increase in repair surgeries have occurred in recent years2. However, in symptomatic patients with irreparable tears, partial meniscectomy remains the standard of care. Meniscectomy is not harmless and can result in increased contact stress, predisposing the patient to early-onset osteoarthritis1.
In a select group of patients with persistent unicompartmental pain and symptomatic meniscus deficiency, meniscal allograft transplantation (MAT) has emerged as an acceptable surgical procedure aiming to restore function and improve pain. In many patients, MAT can result in long-term improvement, with a recent systematic review demonstrating favorable graft survival and functional outcomes at a minimum ten years after surgery3. These favorable outcomes demonstrate lasting symptomatic improvement and, though unproven at this time, may decrease the progression of osteoarthritis in the knee. The purpose of this article is to review five key points on the indications, pre-operative considerations and surgical preparation, surgical technique, and common concomitant procedures of MAT.
Patient Selection
In a specific and finite patient population, MAT can provide significant improvement in pain and function. When considering MAT, it is critical that each patient undergo a thorough history and physical examination to assess candidacy. In the experience of the senior author, there are a number of general indications that should be evaluated when considering surgery4. The goal of this surgery is to predictably reduce pain and improve function and the challenge with older patients is that they often have physiologic osteoarthritis that is unresponsive to the addition of a meniscus. Similarly, BMI is a pro-inflammatory condition in addition to providing additional mechanical loads across the knee that may render a patient less responsive to a meniscus transplant. Thus, with some exceptions, ideally the patient should be younger than fifty years of age with a BMI of less than 355. Surgical history is critical, as any candidate will have undergone previous meniscectomy and ideal candidates should have localized pain limited to the compartment of meniscus deficiency. Patients should also be assessed for normal or correctable limb alignment, ligamentous stability, and articular cartilage status, as inability to correct any of these deficiencies has been associated with inferior outcomes. Another key consideration when assessing surgical candidates is their commitment and willingness to comply with rehabilitation, as any patient following MAT will require months of dedicated physical therapy and rehabilitation to achieve optimal outcomes6. The patient selection criteria utilized by the senior is congruent with the International Meniscus Reconstruction Exports Forum, whose recommendations are shown in Table 15.
Table 1: International Meniscus Reconstruction Experts Forum 2015 Statement on MAT Patient Selection5
| 1. Based on current clinical evidence showing improvements in outcome after MAT, the following are primary indications for MAT: I. Unicompartmental pain in the presence of total or subtotal “functional meniscectomy” II. As a concomitant procedure to revision ACL reconstruction to aid in joint stability when meniscus deficiency is believed to be a contributing factor to failure, III. As a concomitant procedure with articular cartilage repair in a meniscus-deficient compartment. |
| 2. Meniscus deficiency is an indication for MAT; however, it should not be considered as a routine procedure in the asymptomatic patient. |
| 3. When performing an articular cartilage restoration procedure, it is recommended to perform MAT in the absence of a functional meniscus in the involved ipsilateral compartment. |
| 4. Caution should be taken if performing MAT in knees with moderate to severe radiographic OA (i.e. Kellgren-Lawrence grade ≥3) |
Adapted from Getgood et al5
There is significant heterogeneity and controversy regarding contraindications to MAT. Recent studies have highlighted an expanding role for MAT, including a recent evaluation of MAT in patients greater than 50 years old that demonstrated modest yet significant outcome improvement7. However, patients with evidence of diffuse arthritis should be assessed for arthroplasty or other treatment modalities, as any transplanted meniscus would be prone to clinical or surgical failure. An additional source of controversy is whether asymptomatic meniscus-deficient patients should undergo prophylactic MAT, but there is insufficient evidence to treat asymptomatic patients with MAT at this time8.
Graft Selection
Proper selection and sizing of a meniscal allograft is essential in promoting favorable outcomes after MAT. Transplanted meniscus allografts are both size and compartment-specific, and improper graft selection can promote failure of the graft and subsequent need for revision surgery. In particular, mismatch of the graft can lead to graft extrusion, an increasingly recognized cause of failure and revision surgery9,10. Moreover, improper sizing of the graft can lead to increased forces on both the graft and articular cartilage, which in turn can result in advanced rates of degeneration and early failure of the graft11.
To ensure proper sizing of the graft, we utilize the radiographic methods previously outlined by Pollard et al12. Prior to surgery, AP and lateral x-ray imaging of the knee are taken to determine graft measurements. On AP imaging, the distance between the tibial eminence and the periphery of the tibial plateau corresponds to the coronal width of the meniscal graft. When viewing lateral imaging, the AP length of the allograft is calculated as 80 or 70 percent of the AP length of the tibial plateau for medial and lateral allografts, respectively. A modification to the Pollard technique was proposed by Yoon et al, which can also be utilized to calculate precise graft measurements and minimize mismatch13. In addition, recent investigations have demonstrated success in using MRI imaging to precisely size allografts prior to surgery6. However, in our practice, the measurements obtained using the Pollard method alone have been reliably accurate in ensuring proper sizing.
Graft Fixation
There are several different techniques commonly utilized to secure fixation of the meniscal allograft. Generally, fixation techniques can be distinguished as either achieving osseous or soft tissue fixation. Osseous fixation is achieved using either a bone-plug or bone-bridge technique, while soft-tissue fixation can be completed by passing sutures through tibial tunnels or simply with the use of peripheral sutures. All techniques are widely accepted, with no published literature to date identifying a difference in functional outcomes of osseous and soft-tissue fixation6. However, soft-tissue fixation has been found to produce mildly inferior biomechanical outcomes and long-term graft survival rates as compared to osseous fixation14-16. For this reason, as well as increased technical ease when performing any concomitant osteotomy or ligamentous procedure, the preference of the senior author is to use a bridge-in-slot technique for osseous fixation in both medial and lateral MAT.
Graft Preparation and Placement
The bridge-in-slot technique utilized by the senior author has been previously described4,17-19 and is summarized as follows. Following a diagnostic arthroscopy and anterior trans-patellar tendon arthrotomy, attention is made to creating a tibial slot for graft placement. An initial 4.5mm slot is reamed between the anterior and posterior horn insertions. A guidewire is then inserted distal and parallel to the initial slot, which is then overreamed with a 7-8mm cannulated reamer. The final tibial slot is then created using a box cutter, measuring 8mm wide and 10mm deep.
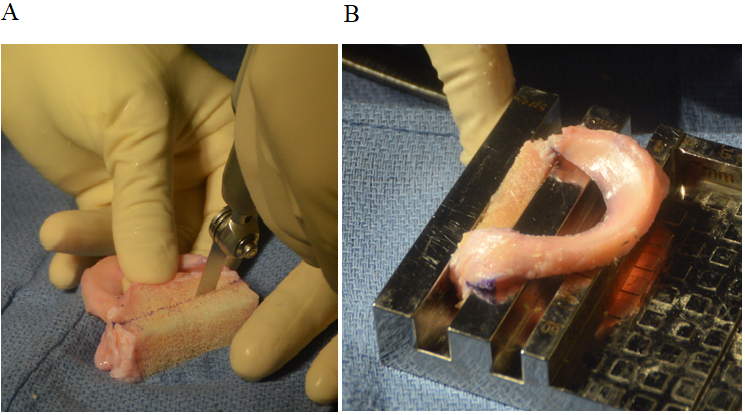
Figure 1A-B: Preparation of allograft bone bridge using donor tibial plateau. Once prepared the bone bridge is sized to ensure a proper fit into the tibial slot.
Graft preparation can be performed once thawed at any time during the case. The allograft tibial plateau is prepared to create the bone bridge, measuring 7mm wide and 10mm deep (Figure 1A-B). A traction stitch is then placed at the junction of the posterior to middle-third of the graft to facilitate graft insertion. Once prepared, the allograft bone bridge is passed into the tibial slot. A passing wire is guided out of the anterior arthrotomy, and the traction stitch on the graft is inserted into the passing wire. The wire is then pulled through an accessory posterolateral or posteromedial incision, and in doing so the graft is inserted into the anterior arthrotomy. Passage of the bone bridge into the tibial slot is then completed under direct visualization, which is then secured using a single interference screw or anchor. Lastly, attention is placed on repairing the meniscus to the joint capsule, which is completed using 8-10 inside-out vertical mattress sutures (Figure 2).
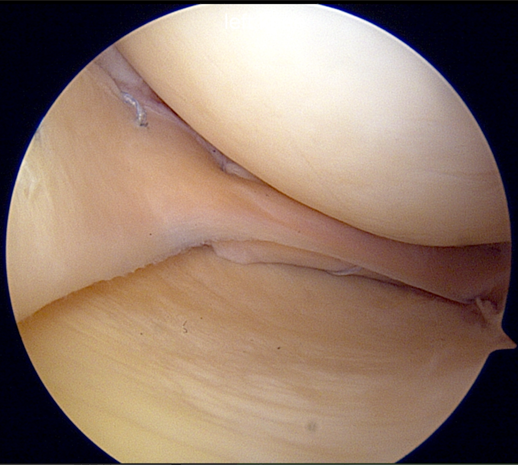
Figure 2: Arthroscopic view of completed meniscus transplantation, with repair of the allograft to native capsule using inside-out sutures.
Concomitant Knee Pathology at the Time of MAT
In each surgical candidate for MAT, it is essential that a detailed history and physical examination be performed to investigate concomitant pathology that is correctable at the time of MAT. In particular, careful attention should be placed on any ligamentous instability or limb misalignment, as in early outcome studies both of these factors were associated with greater rates of MAT failures20,21. In addition, the cartilage status of the patient should be assessed at the time of surgery, as patients with focal chondral defects may benefit from a concomitant cartilage restoration procedure22.
These concomitant procedures may be performed in a staged manner or at the time of MAT. Limb misalignment may be corrected as indicated with either a high tibial osteotomy or a distal femoral osteotomy. In the ACL deficient knee, the preference of the senior author is to perform a modified bridge-in-slot technique as described previously23. In general, any concomitant cartilage procedures or osteotomies should be performed after MAT, as fixation of the meniscal allograft requires significant stress to the knee that may compromise these procedures.
Restoration of normal ligamentous stability and limb alignment should always be achieved, but the presence of focal chondral defects, particularly at the site of meniscus deficiency, presents a significant challenge in identifying the etiology of the patient’s pain as both meniscal and chondral pathologies may play a role. The effect of cartilage status on the long-term outcomes of MAT is well studied and suggests that full-thickness chondral defects do not preclude favorable outcomes and survival rates of MAT24,25. However, the presence of subchondral bone marrow lesions, which often are associated with chondral and/or meniscal deficiency, has been identified as a significant risk factor for inferior outcomes of MAT26. The preference of the senior author is to perform cartilage repair or restoration in Outer bridge grade III or IV defects at the time of MAT. The addition of concomitant osteochondral allograft transplantation or other cartilage preserving procedures at the time of MAT has been investigated, with multiple studies showing comparable outcomes to those receiving isolated MAT22,27.
Conclusion
In young, non-obese patients with minimal osteoarthritis and symptomatic lateral or medial meniscus deficiency, MAT is an established and effective procedure to produce meaningful reductions in pain and significant functional outcome improvements. Careful pre-operative evaluation should be performed in every case to ensure proper sizing of the allograft as well as identification of concomitant injury that can be repaired at the time of surgery. Several different surgical techniques are proven and accepted for completion of MAT, but in our experience the bridge-in-slot osseous fixation technique is preferred.
References
- Rao AJ, Erickson BJ, Cvetanovich GL, et al. The Meniscus-Deficient Knee Biomechanics Evaluation and Treatment Options. Orthop J Sports Med. 2015; 3(10): 2325967115611386.
- Abrams GD, Frank RM, Gupta AK, et al. Trends in meniscus repair and meniscectomy in the United States 2005-2011. Am J Sports Med. 2013; 41(10): 2333-2339.
- Novaretti JV, Patel NK, Lian J, et al. Long-Term Survival Analysis and Outcomes of Meniscal Allograft Transplantation With Minimum 10-Year Follow-Up A Systematic Review. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2019; 35(2): 659-667.
- Frank RM, Cole BJ. Meniscus transplantation. Current reviews in musculoskeletal medicine. 2015; 8(4): 443-450.
- De Bruycker M, Verdonk PCM, Verdonk RC. Meniscal allograft transplantation a meta-analysis. Sicot j. 2017; 3: 33.
- Getgood A, LaPrade RF, Verdonk P, et al. International Meniscus Reconstruction Experts Forum (IMREF) 2015 Consensus Statement on the Practice of Meniscal Allograft Transplantation. Am J Sports Med. 2017; 45(5): 1195-1205.
- Zaffagnini S, Grassi A, Macchiarola L, et al. Meniscal Allograft Transplantation Is an Effective Treatment in Patients Older Than 50 Years but Yields Inferior Results Compared With Younger Patients A Case-Control Study. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2019; 35(8): 2448-2458.
- Frank RM, Yanke A, Verma NN, et al. Immediate Versus Delayed Meniscus Allograft Transplantation Letter to the Editor. The American Journal of Sports Medicine. 2015; 43(5): NP8-NP9.
- Ahn JH, Kang HW, Yang TY, et al. Multivariate Analysis of Risk Factors of Graft Extrusion After Lateral Meniscus Allograft Transplantation. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2016; 32(7): 1337-1345.
- Waterman BR, Rensing N, Cameron KL, et al. Survivorship of Meniscal Allograft Transplantation in an Athletic Patient Population. Am J Sports Med. 2016; 44(5): 1237-1242.
- Brindle T, Nyland J, Johnson DL. The meniscus review of basic principles with application to surgery and rehabilitation. J Athl Train. 2001; 36(2): 160-169.
- Pollard ME, Kang Q, Berg EE. Radiographic sizing for meniscal transplantation. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 1995; 11(6): 684-687.
- Yoon JR, Kim TS, Lim HC, et al. Is Radiographic Measurement of Bony Landmarks Reliable for Lateral Meniscal Sizing? The American Journal of Sports Medicine. 2011; 39(3): 582-589.
- Alhalki MM, Howell SM, Hull ML. How three methods for fixing a medial meniscal autograft affect tibial contact mechanics. Am J Sports Med. 1999; 27(3): 320-328.
- Chen MI, Branch TP, Hutton WC. Is it important to secure the horns during lateral meniscal transplantation? A cadaveric study. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 1996; 12(2): 174-181.
- Paletta GA Jr, Manning T, Snell E, et al. The effect of allograft meniscal replacement on intraarticular contact area and pressures in the human knee. A biomechanical study Am J Sports Med. 1997; 25(5): 692-698.
- Cole BJ, Carter TR, Rodeo SA. Allograft meniscal transplantation background techniques and results. Instructional course lectures. 2003; 52: 383-396.
- Cole BJ, Dennis MG, Lee SJ, et al. Prospective evaluation of allograft meniscus transplantation a minimum 2-year follow-up. Am J Sports Med. 2006; 34(6): 919-927.
- Mascarenhas R, Yanke AB, Frank RM, et al. Meniscal allograft transplantation: preoperative assessment surgical considerations and clinical outcomes. The journal of knee surgery. 2014; 27(6): 443-458.
- Cameron JC, Saha S. Meniscal allograft transplantation for unicompartmental arthritis of the knee. Clinical orthopaedics and related research. 1997; 337: 164-171.
- van Arkel ER, de Boer HH. Human meniscal transplantation. Preliminary results at 2 to 5-year follow-up. The Journal of bone and joint surgery British volume. 1995; 77(4): 589-595.
- Frank RM, Lee S, Cotter EJ, et al. Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation A Comparative Matched Group Analysis. Am J Sports Med. 2018; 46(3): 573-580.
- Saltzman BM, Griffin JW, Wetters N, et al. Concomitant Arthroscopic Meniscal Allograft Transplantation and Anterior Cruciate Ligament Reconstruction. Arthroscopy techniques. 2016; 5(5): e1161-e1171.
- Mahmoud A, Young J, Bullock-Saxton J, et al. Meniscal Allograft Transplantation The Effect of Cartilage Status on Survivorship and Clinical Outcome. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2018; 34(6): 1871-1876.e1871.
- Saltzman BM, Meyer MA, Leroux TS, et al. The Influence of Full-Thickness Chondral Defects on Outcomes Following Meniscal Allograft Transplantation A Comparative Study. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2018; 34(2): 519-529.
- Saltzman BM, Cotter EJ, Stephens JP, et al. Preoperative Tibial Subchondral Bone Marrow Lesion Patterns and Associations With Outcomes After Isolated Meniscus Allograft Transplantation. The American Journal of Sports Medicine. 2018; 46(5): 1175-1184.
- Harris JD, Cavo M, Brophy R, et al. Biological knee reconstruction a systematic review of combined meniscal allograft transplantation and cartilage repair or restoration. Arthroscopy the journal of arthroscopic & related surgery official publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 2011; 27(3): 409-418.
