Subtalar and Chopart Dislocations in Children and Adolescents
N. K. Sferopoulos
Department of Pediatric Orthopaedics, “G. Gennimatas” Hospital, Thessaloniki, Greece
Abstract
Subtalar and Chopart dislocations are extremely rare in childhood but become slightly more common in older children and adolescents. Subtalar dislocation involves dislocation of the subtalar and talonavicular joints, with intact tibiotalar and calcaneocuboid joints, in the absence of a talar neck fracture. It should be differentiated from the Chopart dislocation and from traumatic entities presenting radiographically as isolated talonavicular dislocations. Chopart joint injury involves the talonavicular and calcaneocuboid joints of the foot. The injury may appear as sprain, fracture, subluxation or dislocation. Diagnosis is made on plain radiographs; although initial views may not reveal the severity of the lesion, since spontaneous reduction may occur. The radiographic detection of an isolated talonavicular dislocation is probably indicative of a Chopart joint injury, in which a momentary subluxation or dislocation of the calcaneocuboid joint has occurred. The differential diagnosis of a radiographically detected isolated talonavicular dislocation should also include traumatic entities associated with intact calcaneocuboid joint, such as the swivel talonavicular dislocation and the isolated displacement of only the medial part of the Chopart joint. The swivel talonavicular dislocation is a subtype of the Chopart joint injury, in which the foot with the calcaneus is rotated beneath the talus, producing subtalar subluxation but not dislocation. In the isolated displacement of only the medial part of the Chopart joint the subtalar joint is not injured. The injury is usually associated with a fracture of the body of the tarsal navicular and it is believed to be the result of severe abduction or adduction of the forefoot.
Subtalar dislocations and Chopart joint injuries in children and adolescents seem to be comparable with their adult counterparts in the mechanism of injury, classification, treatment, complications and outcome. The challenges in treating these injuries are to achieve adequate diagnosis and prompt treatment. It appears mandatory that obtaining and maintaining an early anatomic reduction remains the key factor in achieving good outcomes. However, a high incidence of complications, such as compartment syndrome, soft tissue compromise, avascular necrosis of bone, bone growth deformities and debilitating early post-traumatic arthritis, have been reported.
The purpose of this report is to review the relevant publications on subtalar and Chopart dislocations in children and adolescents and to present illustrative cases treated at our institution.
Review
In the last decades, foot injuries in children and adolescents have presented an increase in prevalence and severity. A careful clinical evaluation is an indispensable prerequisite for the identification of subtalar dislocations and Chopart joint injuries. The plantar ecchymosis sign implies the potential for significant injury of the hind- or midfoot (Fig. 1). Compartment syndrome must be ruled out through direct pressure measurements, particularly in unconscious patients. Significant malalignment may be overlooked without the plain standard anteroposterior, lateral and oblique radiographs of the injured foot. Subsequently, additional imaging may also be required. Radiographs taken with the patient weight bearing are useful to diagnose a subtle or unstable injury; stress radiographs with the patient under anesthesia are also useful if there is clinical suspicion of injury despite unremarkable radiographs; computed tomography is valuable for assessing intraarticular osteochondral fragments, occult fractures, to access the congruency after closed reduction and to aid preoperative surgical planning, while magnetic resonance imaging is useful to detect ligamentous or osteochondral lesions and bone bruising. The treatment decision requires individual consideration and it is usually based on the full extent of the lesions, considering the number of affected foot regions (ankle, talus, calcaneus, Chopart joint, Lisfranc joint, mid- and forefoot), as well as on the degree of soft tissue injury (open or closed lesion). An early closed reduction under sedation, analgesia, and muscle relaxation should be attempted in closed injuries. Internal fixation may be maintained with percutaneous smooth pins in cases with instability. This technique is much simpler than external fixation for both the patient and surgeon. Open reduction may be required in closed cases with an incongruent reduction and in open lesions. The limb should be immobilized in a plaster splint and in a circumferential non-weight-bearing below-knee cast, as soon as edema subsides, for approximately 6 weeks to allow for soft tissue healing, after either closed or open treatment modalities. Strengthening exercises and progressive weight bearing as tolerated may follow for up to 3 months. Recently, shorter periods of immobilization have been advocated to avoid joint stiffness1-24.
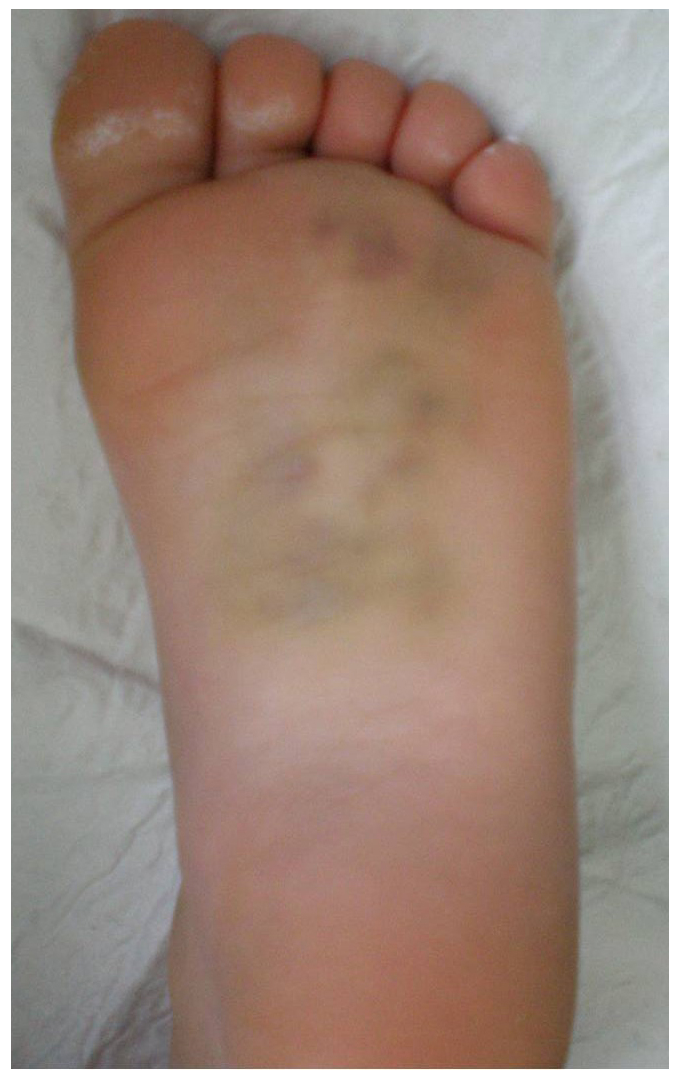
Figure 1: The plantar ecchymosis sign was detected in a 7-year-old girl. She was injured when a car drove over her foot. She presented with inability to bear weight as well as pain, diffuse swelling and local tenderness. Initial radiographs indicated no fracture. MRI revealed multifocal bone bruising of the tarsal bones (From Sferopoulos24).
Subtalar dislocation defines the simultaneous dislocation of the subtalar (talocalcaneal) and talonavicular joints without associated injury of the tibiotalar (talocrural or ankle joint) or calcaneocuboid joints and without talar neck fracture. The lesion has been alternatively termed peritalar, subtalus, subastragalar, subastrag(a)loid, hindfoot and talocalcaneonavicular dislocation.
The peritalar anatomic structures include the distal tibia and fibula, calcaneus, navicular and cuboid as well as their articulations and their stabilizing ligaments. The subtalar, the talonavicular and the calcaneocuboid joints, function as a unit to invert and evert the foot. Peritalar subluxations or dislocations may involve one or more of the peritalar articulations. Therefore, apart from subtalar dislocations, tibiotalar, talonavicular, Chopart joint, Chopart joint/subtalar (all hindfoot joints) and total or complete talar (pantalar) dislocations may also be defined as peritalar. Isolated dislocation of a single peritalar joint is unusual. A radiographically isolated midtarsal, talonavicular or calcaneocuboid, dislocation is most probably associated with radiographically undetectable ligamentous disruption of the adjoining articulations of the hind- or midfoot and/or various fractures of the foot.
After DuFaurest and Judcy reports in 1811, Broca, in 1853, and Malgaigne, in 1856, suggested a purely anatomic classification, describing in descending order of frequency, medial (79.5%), lateral (17%), posterior or plantar (2.5%) and anterior or dorsal (1%) subtalar dislocations. These types refer to the forces applied to a plantar-flexed foot either in inversion, resulting in medial dislocation, or eversion, resulting in lateral dislocation. The medial dislocation is sometimes referred to as an “acquired clubfoot” or “basketball foot”, while the lateral dislocation is sometimes referred to as an “acquired flatfoot”. The normal longitudinal axis of the foot is maintained and the deformity is much less pronounced in pure posterior or anterior dislocations. The mechanism of injury has been classified as direct or indirect. Direct injuries are usually high-energy injuries commonly due to motor vehicle accidents or falls from a height. Indirect injuries are usually low-energy injuries commonly due to sporting activities, such as a simple inversion injury of the foot while playing basketball. Lateral dislocations are usually due to higher-energy trauma and are often associated with open injuries, associated fractures, neurovascular compromise and poor results. The injury is very rare in childhood considering the greater elasticity of bone in children, while the open physeal plates of the distal tibia and fibula are believed to act as the path of least resistance, fracturing prior to the occurrence of a subtalar dislocation. The diagnosis is usually obvious on standard anteroposterior, lateral and oblique views of the foot or ankle but it may be easily missed in the polytrauma patient. Postreduction radiographs are essential to confirm a stable anatomic reduction and to identify additional fractures. Subtalar dislocations are frequently associated with concomitant fractures, including intraarticular osteochondral fractures, occurring in 12-38% of medial and up to 100% of lateral dislocations. The radiographic detection of these fractures, most commonly of the medial and lateral tubercles of the posterior process of the talus, may indicate the potential diagnosis of a more subtle subtalar injury. The majority of closed subtalar dislocations in children and adolescents can be reduced in a closed fashion, as in adults. Indications for open reduction and possibly internal fixation with smooth Kirshner wires or Steinmann pins of a closed subtalar dislocation include residual subtalar or talonavicular instability, inability to achieve a congruent reduction, and the need for open treatment of associated intraarticular fractures. Open injuries require débridement, open reduction, and have the same indications for temporary joint or bone transfixion. Common blocks to reduction for medial dislocations include an interposed extensor retinaculum or extensor digitorum brevis and talonavicular impaction fractures, while for lateral dislocations an interposed posterior tibial, anterior tibial, peroneal, flexor hallucis or digitorum longus tendon, interposed joint capsules and obstructing fracture fragments. With prompt treatment and early mobilization, children and adolescents with closed, simple subtalar dislocations may expect a favorable long-term prognosis, with little to no residual disability. An impaction fracture of the talonavicular joint is the most consistent finding adversely affecting outcome in pediatric subtalar dislocations, according to Dimentberg and Rosman, since inadequate or lost reduction may be evident and remodeling is not expected. Delayed diagnosis, misdiagnosis, failure to reduce the dislocation promptly, irreducible dislocations, open dislocations, high-energy injuries, polytrauma, intraarticular fractures and prolonged immobilization are usually associated with a poor outcome25-72.
The Chopart joint, also known as the transverse tarsal or midtarsal joint is formed by the articulations of the talus with the navicular (talocalcaneonavicular or commonly called talonavicular joint) and of the calcaneus with the cuboid (calcaneocuboid joint). The talonavicular joint is more vulnerable to injuries, as part of the more elastic medial column, while the calcaneocuboid joint, forming part of the rigid lateral column, is more stable due to its saddle shape, to the strong capsuloligamentous structures and to its close proximity to the peroneus longus tendon. Studies in adults have shown that, in the midtarsal joint injuries, compression fracture of a column is usually associated with instability or avulsion fracture in the contralateral column as well. The causes of midtarsal joint injuries are variable. They may be subdivided into the, most common, low-energy midtarsal subtle sprains or subluxations and the, relatively rare, high-energy Chopart fracture and/or dislocations. In adults, the incidence of Chopart sprains ranges up to one-third of patients experiencing lateral ankle sprains, due to a similar mechanism of trauma and comparable clinical symptoms, as a result of the proximity of the lateral collateral ankle ligaments and the lateral Chopart joint ligaments. The mechanism of injury has been classified as either direct or indirect. In direct injuries the force is applied directly to the Chopart joint, as with crush injuries, fall from a height, falling objects and traffic collisions, while indirect injuries result from a combination of twisting and axial-loading of the foot, as seen in sports-related trauma. Midtarsal joint injuries have been classified by Main and Jowett, in 1975, according to the direction of the deforming force applied to the midfoot at the time of injury. The classification scheme consists of five patterns of injury resulting from medial forces, longitudinal forces, lateral forces, plantar forces and crush injuries. Review of the crush midtarsal injury pattern is more appropriate as a fracture than a dislocation. Medial and dorsal displacement of the Chopart joint, occurring when the foot is plantar flexed and inverted, is the most typical type of dislocation. Dislocations with lateral displacement, occurring during eversion injuries, are normally the result of higher-energy trauma and have a worse prognosis due to the increased frequency of open injuries and associated fractures. Most patients with Chopart joint injury may suffer from radiographically undetectable concomitant injuries of the subtalar or Lisfranc joints as well as fractures of the hind- and midfoot. The unstable painful midfoot deformity is usually apparent on the physical examination of the traumatized patient, but it may occasionally be masked by severe early swelling and ecchymosis. Diagnosis is usually based on the plain radiographs of the foot, although the extent of injury is often underestimated. Isolated fractures and/or dislocations of either the medial or the lateral part of the Chopart joint are extremely rare injuries. The calcaneocuboid dislocation may often be transient and radiographically undetectable. The calcaneocuboid injury is generally resulting in less displacement than at the talonavicular joint, but joint space widening may occasionally be radiographically evident instead. Impaction injuries as well as avulsion injuries of the Chopart joint-spanning ligaments may be easily overlooked on radiographs. Avulsion fractures across the Chopart joint, especially of the anterior calcaneal process and the dorsal talonavicular joint, have been well recognized as strong indication of Chopart joint injury and midtarsal sprain. Recent literature states the rate of misdiagnosis to be up to 55% in adults. Pediatric orthopaedic surgeons should be aware that a high index of clinical suspicion is required for early diagnosis. However, additional to radiographs imaging evaluation should be reserved only for patients in whom the clinical diagnosis is unclear or who have symptoms disproportionate to the radiographic findings. Emergent neurovascular complications of the foot should be excluded before attempting reduction. Treatment comprises early stable anatomic reduction of the injury. Surgical reduction and fixation is primarily indicated in Chopart joint injuries with a delayed diagnosis and interposed soft tissue or osseous structures. High-energy, open or severely displaced injuries, associated fractures, disability to diagnose the injury promptly or restore anatomic articular congruity and foot alignment worsen the outcome73-101.
Two unique mechanisms of injury, the medial and lateral swivel dislocation, have been included in the classification of Chopart joint injuries proposed by Main and Jowett. They result in isolated talonavicular dislocation from medial or lateral directed force applied to the midfoot, respectively, without complete disruption of the talocalcaneal ligaments and with an intact calcaneocuboid joint. The injuries result from a type of tarsal rotation or swivel injury, without inversion or eversion of the foot. A medially directed force causes compression at the talonavicular joint with distraction at the calcaneocuboid joint. A laterally directed force causes compressive forces at the calcaneocuboid joint with distraction at the talonavicular joint. The lesions have also been defined as an uncommon special type of either medial or lateral Chopart joint stress injury. In addition, swivel dislocation has been presented as an uncommon variant of subtalar dislocation in which the talonavicular dislocation is associated with subluxation, but not dislocation, of the subtalar joint. The axis of rotation in swivel injuries is through the intact calcaneocuboid joint or the intact interosseous talocalcaneal ligament. The latter is in contrast with the more common occurrence in which this ligament ruptures, allowing subtalar dislocation. The lesions may present with little clinical evidence of malalignment and they can be easily missed both clinically and radiographically. The isolated talonavicular joint, medial or lateral, incongruity may be the only detected radiographic joint abnormality in swivel injuries. The talonavicular joint injury may appear as total disruption or, more commonly, as partial subluxation. Subtalar subluxation may be radiographically evident due to the calcaneus rotation or swivel, on the intact interosseous talocalcaneal ligament in the sinus tarsi, beneath the talus, taking with it the cuboid. A wide variety of ankle or foot fractures have been recorded in the reported patients with swivel dislocations, which have all been detected in adults with a minimum age of 18 years102-119.
A traumatic entity that may be easily confused with swivel dislocation is the rare isolated talonavicular dislocation associated with a displaced fracture of the body of the tarsal navicular, when no subtalar subluxation or dislocation and no injury to the calcaneocuboid joint have occurred. This injury is believed to be the result of severe abduction or adduction of the forefoot, rather than the previously described tarsal rotation or swivel injury. The isolated displacement, usually medial, of the talonavicular dislocation is the only detected radiographic abnormality involving the peritalar joints120-122. Isolated talonavicular dislocations have been reported in adults in conjunction with a wide variety of ipsilateral foot fractures123-128.
In conclusion, the differential diagnosis of an isolated talonavicular dislocation, especially when it is associated with a fractured body of the tarsal navicular, from a subtalar or a Chopart joint injury, including a swivel dislocation, cannot be solely based on the findings of the radiographic investigation (Fig. 2). It may be prudent to consider that this traumatic entity should be primarily considered as an occult Chopart joint injury unless additional, to plain radiographs, imaging findings prove no injury to the calcaneocuboid articulation and ligaments, and no bone bruising of the adjacent subchondral bone.
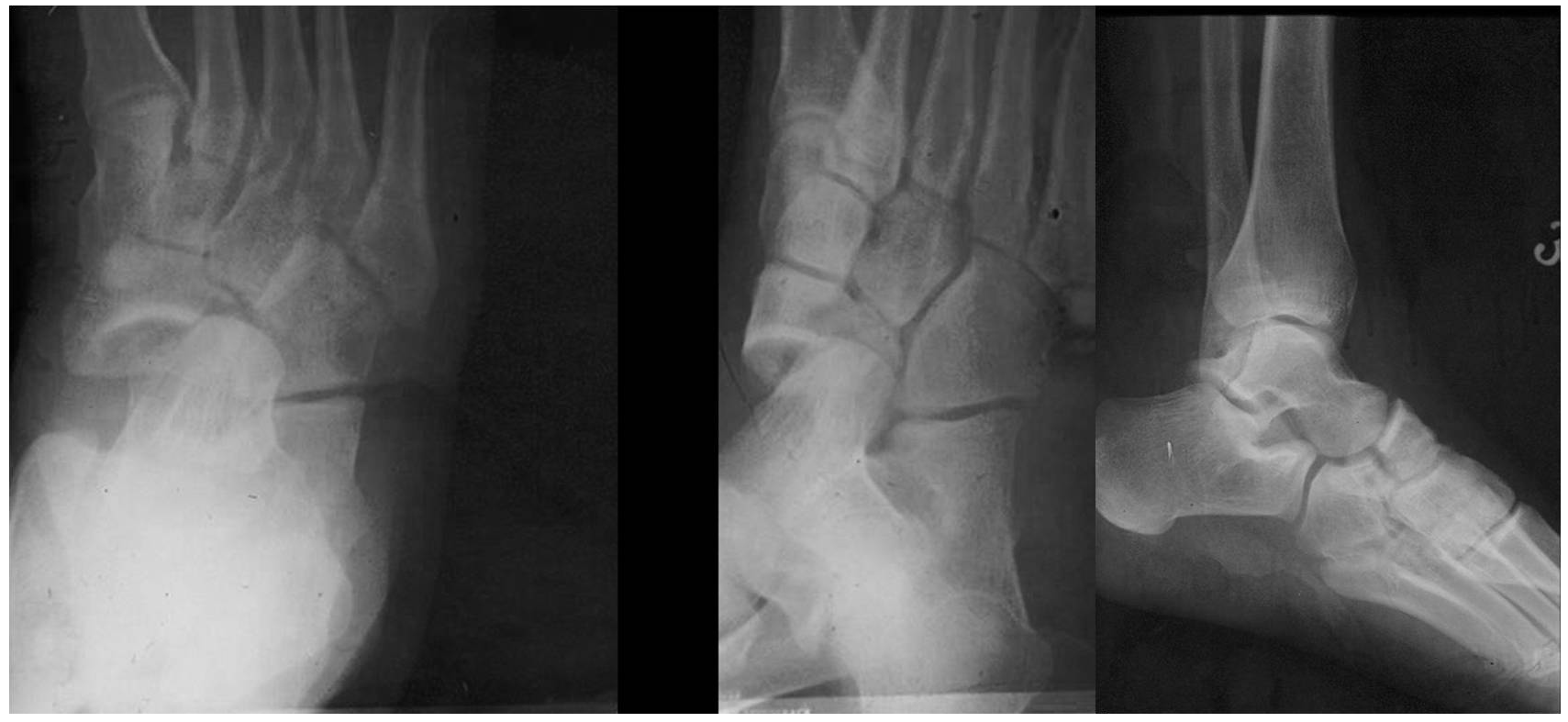
Figure 2: A 15-year-old-girl suffered a closed injury of her foot caused by a horse fall. Initial radiographs revealed an isolated talonavicular dislocation with medial displacement and a navicular fracture. There was no evidence of an impaction fracture at the Chopart joint. Both the subtalar and calcaneocuboid joints showed no radiographic abnormality. The distal navicular articulation (naviculocuneiform) also appeared normal. The fracture-dislocation of the talonavicular joint indicates that a momentary subluxation or dislocation of the calcaneocuboid joint should be seriously considered. However, a secure diagnosis of a Chopart joint injury may not be established solely on the radiographic appearance. A subtalar dislocation, a medial swivel dislocation as well as an isolated talonavicular dislocation associated with a tarsal navicular fracture should also be included in the differential diagnosis. There was no evidence of neurovascular compromise. Closed manipulative reduction of the dislocation was successfully performed under general anesthesia with additional muscle relaxation. Postreduction and cast immobilization radiographs for eight weeks confirmed stability of the talonavicular joint and satisfactory reduction of the navicular fracture.
References
- Tomaschewski HK. Results in the treatment of post-traumatic growth abnormalities of the foot in children and adolescents. Beitr Orthop Traumatol. 1975; 22(2): 90. PMID: 1218040
- Ehrensperger J. Fractures of the foot in children and adolescents. Ther Umsch. 1983; 40(11): 996-1000. PMID: 6140773
- Linhart WE, Höllwarth ME. Fractures of the child’s foot. Orthopade. 1986; 15(3): 242-50. PMID: 2874539
- Suren EG, Zwipp H. Acute ligamentous injuries of the Chopart and Lisfranc joint line. Orthopade. 1986; 15(6): 479-86. PMID: 3808709
- Zwipp H, Ranft T. Malunited juvenile fractures in the foot region. Orthopade. 1991; 20(6): 374-80. PMID: 1684652
- DeLee JC. Fractures and dislocations of the foot. In: Mann RA, Coughlin MJ, eds. Surgery of the foot and ankle. 6th ed. St. Louis: MO: Mosby; 1992.
- Rockwood CA Jr, Wilkins KE, Beaty JH. Fractures in children. 4th ed. Philadelphia: Lippincott-Raven Publishers; 1996.
- Loder RT, Brown KL, Zaleske DJ, et al. Extremity lawn-mower injuries in children: Report by the Research Committee of the Pediatric Orthopaedic Society of North America. J Pediatr Orthop. 1997; 17(3): 360-9. PMID: 9150027
- Thermann H, Schratt HE, Hufner T, et al. Fractures of the pediatric foot. Unfallchirurg. 1998; 101(1): 2-11. PMID: 9522665 DOI: 10.1007/s001130050225
- Ogden JA. Skeletal injury in the child. 3rd ed. New York: Springer Verlag; 2000.
- Kay RM, Tang CW. Pediatric foot fractures: evaluation and treatment. J Am Acad Orthop Surg. 2001; 9: 308-19. PMID: 11575910 DOI: 10.5435/00124635-200109000-00004
- Crawford AH, Al-Sayyad MJ. Fractures and dislocations of the foot and ankle. In: Green NE, Swiontkowski MF, eds. Skeletal trauma in children. Philadelphia: Saunders; 2003.
- Wagner R, Blattert TR, Weckbach A. Talar dislocations. Injury. 2004; 35 Suppl 2: SB36-45. PMID: 15315877 DOI: 10.1016/j.injury.2004.07.010
- Ribbans WJ, Natarajan R, Alavala S. Pediatric foot fractures. Clin Orthop Relat Res. 2005; 432: 107-15. PMID: 15738810 DOI: 10.1097/01.blo.0000156451.40395.fc
- Mayr J, Peicha G, Grechenig W, et al. Fractures and dislocations of the foot in children. Clin Podiatr Med Surg. 2006; 23(1): 167-89, ix. PMID: 16598914 DOI: 10.1016/j.cpm.2005.10.011
- Grivas TB, Vasiliadis ED, Koufopoulos G, et al. Midfoot fractures. Clin Podiatr Med Surg 2006; 23(2): 323-41, vi. PMID: 16903156 DOI: 10.1016/j.cpm.2006.01.001
- Fernandez Fernandez F. Fractures and dislocations of the foot. In: Benson M, Fixsen J, Macnicol M, Parsch K, eds. Children’s orthopaedics and fractures. 3rd ed. London: Springer-Verlag; 2010.
- McCarthy JJ, Ganley TJ, Herman M, et al. Fractures of the foot in children and adolescents. In: McCarthy JJ, Drennan JC, eds. Drennan’s the child’s foot and ankle. 2nd ed. Philadelphia: Lippincott Williams & Wilkins; 2010.
- Eberl R, Ruttenstock EM, Singer G, et al. Treatment algorithm for complex injuries of the foot in paediatric patients. Injury. 2011; 42(10): 1171-8. PMID: 22081809 DOI: 10.1016/j.injury.2009.08.005
- Rammelt S, Schneiders W, Fitze G, et al. Foot and ankle fractures in children. Orthopade. 2013; 42(1): 45-54.
- Benirschke SK, Meinberg EG, Anderson SA, et al. Fractures and dislocations of the midfoot: Lisfranc and Chopart injuries. Instr Course Lect. 2013; 62: 79-91. PMID: 23395016
- Sferopoulos NK. Residual symptoms of occult pediatric ankle injuries: MRI-diagnosed bone bruising. British Journal of Medicine & Medical Research 2014; 4(1): 295-303. DOI: 10.9734/BJMMR/2014/5607
- Rammelt S, Godoy-Santos AL, Schneiders W, et al. Foot and ankle fractures during childhood: Review of the literature and scientific evidence for appropriate treatment. Rev Bras Ortop. 2016; 51(6): 630-9. PMID: 28050532 DOI: 10.1016/j.rboe.2016.09.001
- Sferopoulos NK. Talus fractures in children. ARC Journal of Research in Sports Medicine. 2017; 2(1): 21-6.
- Shands AR Jr. The incidence of subastragaloid dislocation of the foot with a report of one case of the inward type. J Bone Joint Surg Am. 1928; 10: 306-13.
- Leitner B. Obstacles to reduction in subtalar dislocations. J Bone Joint Surg Am. 1954; 36: 299-306. PMID: 13152139
- Barber JR, Bricker JD, Haliburton RA. Peritalar dislocation of the foot. Can J Surg. 1961; 4: 205-10.PMID: 13686767
- Christensen SB, Lorentzen JE, Krogsoe O, et al. Subtalar dislocation. Acta Orthop Scand. 1977; 48(6): 707-11. PMID: 607761 DOI: 10.3109/17453677708994821
- DeLee JC, Curtis R. Subtalar dislocation of the foot. J Bone Joint Surg Am. 1982; 64(3): 433-7. PMID: 7061560
- Zimmer TJ, Johnson KA. Subtalar dislocations. Clin Orthop Relat Res. 1989; 238: 190-4. PMID: 2910600
- Freund KG. Subtalar dislocations: A review of the literature. J Foot Surg. 1989; 28(5): 429-32. PMID: 2685089
- Dimentberg R, Rosman M. Peritalar dislocations in children. J Pediatr Orthop. 1993; 13(1): 89-93. PMID: 8416362 DOI: 10.1097/01241398-199301000-00018
- Sarrafian SK. Biomechanics of the subtalar joint complex. Clin Orthop Relat Res. 1993; 290: 17-26. PMID: 8472445
- Ebraheim NA, Skie MC, Podeszwa DA. Medial subtalar dislocation associated with fracture of the posterior process of the talus. A case report. Clin Orthop Relat Res. 1994; 303: 226-30.PMID: 8194238
- Chen YJ, Hsu RW. Fracture of the posterior process of the talus associated with subtalar dislocation: Report of a case. J Formos Med Assoc. 1994; 93(9): 802-5. PMID: 7735011
- Goldner JL, Poletti SC, Gates HS 3rd, et al. Severe open subtalar dislocations. Long-term results. J Bone Joint Surg Am. 1995; 77(7): 1075-9. PMID: 7608231 DOI: 10.2106/00004623-199507000-00015
- Naranja RJ Jr, Monaghan BA, Okereke E, et al. Open medial subtalar dislocation associated with fracture of the posterior process of the talus. J Orthop Trauma. 1996; 10(2): 142-4. PMID: 8932677 DOI: 10.1097/00005131-199602000-00014
- Bohay DR, Manoli A 2nd. Occult fractures following subtalar joint injuries. Foot Ankle Int. 1996; 17(3): 164-9. PMID: 8919622 DOI: 10.1177/107110079601700309
- Gross RH. Fractures and dislocations of the foot. In: Rockwood CA, Wilkins KE, King RE, eds. Rockwood and Green’s: Fractures in children. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 1996.
- Saltzman C, Marsh JL. Hindfoot Dislocations: When are they not benign? J Am Acad Orthop Surg. 1997; 5(4): 192-8. PMID: 10797221 DOI: 10.5435/00124635-199707000-00002
- Bibbo C, Lin SS, Abidi N, et al. Missed and associated injuries after subtalar dislocation: The role of CT. Foot Ankle Int. 2001; 22(4): 324-8. PMID: 11354446 DOI: 10.1177/107110070102200409
- Bibbo C, Anderson RB, Davis WH. Injury characteristics and the clinical outcome of subtalar dislocations: A clinical and radiographic analysis of 25 cases. Foot Ankle Int. 2003; 24(2): 158-63. PMID: 12627624 DOI: 10.1177/107110070302400210
- Dougherty CP, Nebergall RW, Caskey PM. Lateral subtalar dislocation in a 19-month-old female. Am J Orthop (Belle Mead NJ). 2003; 32(12): 598-600.PMID: 14713066
- Ledoux WR, Sangeorzan BJ. Clinical biomechanics of the peritalar joint. Foot Ankle Clin. 2004; 9(4): 663-83, v. PMID: 15498699 DOI: 10.1016/j.fcl.2004.06.005
- Piazza SJ. Mechanics of the subtalar joint and its function during walking. Foot Ankle Clin. 2005; 10(3): 425-42, v. PMID: 16081013 DOI: 10.1016/j.fcl.2005.04.001
- Giuliani JR, Freedman BA, Shawen SB, et al. Subtalar dislocation in an 8-year-old boy: A rare clinical presentation. Am J Orthop (Belle Mead NJ). 2007; 36(3): 148-51. PMID: 17461397
- de Palma L, Santucci A, Marinelli M, et al. Clinical outcome of closed isolated subtalar dislocations. Arch Orthop Trauma Surg. 2008; 128(6): 593-8. PMID: 17909825 DOI: 10.1007/s00402-007-0459-8
- Kou JX, Fortin PT. Commonly missed peritalar injuries. J Am Acad Orthop Surg. 2009; 17(12): 775-86. PMID: 19948702 DOI: 10.5435/00124635-200912000-00006
- Horning J, DiPreta J. Subtalar dislocation. Orthopedics. 2009; 32(12): 904. PMID: 20000242 DOI: 10.3928/01477447-20091020-17
- Weindel S, Schmidt R, Rammelt S, et al. Subtalar instability: A biomechanical cadaver study. Arch Orthop Trauma Surg. 2010; 130(3): 313-9. PMID: 18839193 DOI: 10.1007/s00402-008-0743-2
- Jungbluth P, Wild M, Hakimi M, et al. Isolated subtalar dislocation. J Bone Joint Surg Am. 2010; 92(4): 890-4. PMID: 20360512 DOI: 10.2106/JBJS.I.00490
- Lasanianos NG, Lyras DN, Mouzopoulos G, et al. Early mobilization after uncomplicated medial subtalar dislocation provides successful functional results. J Orthop Traumatol. 2011 Mar; 12(1): 37-43. PMID: 21308390 DOI: 10.1007/s10195-011-0126-2
- Liu Z, Zhao Q, Zhang L. Medial subtalar dislocation associated with fracture of the posterior process of the talus. J Pediatr Orthop B. 2012; 21(5): 439-42. PMID: 22331059 DOI: 10.1097/BPB.0b013e328351419c
- Karampinas PK, Kavroudakis E, Polyzois V, et al. Open talar dislocations without associated fractures. Foot Ankle Surg. 2014; 20(2): 100-4. PMID: 24796827 DOI: 10.1016/j.fas.2013.12.005
- Jastifer JR, Gustafson PA. The subtalar joint: Biomechanics and functional representations in the literature. Foot (Edinb). 2014; 24(4): 203-9. PMID: 25175840 DOI: 10.1016/j.foot.2014.06.003
- Apostle KL, Coleman NW, Sangeorzan BJ. Subtalar joint axis in patients with symptomatic peritalar subluxation compared to normal controls. Foot Ankle Int. 2014; 35(11): 1153-8. PMID: 25104749 DOI: 10.1177/1071100714546549
- Berkowitz MJ, Sanders RW. Dislocations of the foot. In: Coughlin MJ, Saltzman CL, Anderson RB, eds. Mann's surgery of the foot and ankle. 9th ed. Philadelphia: Elsevier Saunders; 2014.
- Rammelt S, Goronzy J. Subtalar dislocations. Foot Ankle Clin. 2015; 20(2): 253-64. PMID: 26043242 DOI: 10.1016/j.fcl.2015.02.008
- Maceira E, Monteagudo M. Subtalar anatomy and mechanics. Foot Ankle Clin. 2015; 20(2): 195-221. PMID: 26043239 DOI: 10.1016/j.fcl.2015.02.001
- Melenevsky Y, Mackey RA, Abrahams RB, et al. Talar fractures and dislocations: A radiologist's guide to timely diagnosis and classification. Radiographics. 2015; 35(3): 765-79. PMID: 25969933 DOI: 10.1148/rg.2015140156
- Park CH, Park KH. Fracture of the posterior process of the talus with concomitant subtalar dislocation. J Foot Ankle Surg. 2016; 55(1): 193-7. PMID: 26213161 DOI: 10.1053/j.jfas.2015.05.006
- Hui SH, Lui TH. Anterior subtalar dislocation with comminuted fracture of the anterior calcaneal process. BMJ Case Rep. 2016; 2016: bcr2015213835. PMID: 26887882 DOI: 10.1136/bcr-2015-213835
- Prada-Canizares A, Aunon-Martin I, Vila Y Rico J, et al. Subtalar dislocation: Management and prognosis for an uncommon orthopaedic condition. Int Orthop. 2016; 40(5): 999-1007. PMID: 26208589 DOI: 10.1007/s00264-015-2910-8
- Ruhlmann F, Poujardieu C, Vernois J, et al. Isolated acute traumatic subtalar dislocations: Review of 13 cases at a mean follow-up of 6 years and literature review. J Foot Ankle Surg. 2017; 56(1): 201-7.PMID: 26947001 DOI: 10.1053/j.jfas.2016.01.044
- Banerjee S, Abousayed MM, Vanderbrook DJ, et al. Lateral subtalar dislocation with tarsometatarsal dislocation: A case report of a rare injury. Case Rep Orthop. 2017; 2017: 8090721. PMID: 28761771 DOI: 10.1155/2017/8090721
- Bartonicek J, Rammelt S, Nanka O. Anatomy of the subtalar joint. Foot Ankle Clin. 2018; 23(3): 315-40. PMID: 30097077 DOI: 10.1016/j.fcl.2018.04.001
- Sangeorzan A, Sangeorzan B. Subtalar joint biomechanics: From normal to pathologic. Foot Ankle Clin. 2018; 23(3): 341-52. PMID: 30097078 DOI: 10.1016/j.fcl.2018.04.002
- Rammelt S, Bartonicek J, Park KH. Traumatic injury to the subtalar joint. Foot Ankle Clin. 2018; 23(3): 353-74. PMID: 30097079 DOI: 10.1016/j.fcl.2018.04.004
- Mittlmeier T, Rammelt S. Update on subtalar joint instability. Foot Ankle Clin. 2018; 23(3): 397-413. PMID: 30097081 DOI: 10.1016/j.fcl.2018.04.005
- Flippin M, Fallat LM. Open talar neck fracture with medial subtalar joint dislocation: A case report. J Foot Ankle Surg. 2019; 58(2): 392-7. PMID: 30658956 DOI: 10.1053/j.jfas.2018.08.049
- Pena Fernandez M, Hoxha D, Chan O, et al. Centre of rotation of the human subtalar joint using weight-bearing clinical computed tomography. Sci Rep. 2020; 10(1): 1035. PMID: 31974489 DOI: 10.1038/s41598-020-57912-z
- Arain AR, Adams CT, Haddad SF, et al. Diagnosis and treatment of peritalar injuries in the acute trauma setting: A review of the literature. Adv Orthop. 2020; 2020:1852025. PMID: 31984140 DOI: 10.1155/2020/1852025
- Elftman H. The transverse tarsal joint and its control. Clin Orthop. 1960; 16(16): 41-6. PMID: 13819895
- Dewar FP, Evans DC. Occult fracture-subluxation of the midtarsal joint. J Bone Joint Surg Br. 1968; 50(2): 386-8. PMID: 4385043
- Stark WA. Occult fracture-subluxation of the midtarsal joint. Clin Orthop Relat Res. 1973; 93: 291-2. PMID: 4722954 DOI: 10.1097/00003086-197306000-00033
- Howie CR, Hooper G, Hughes SP. Occult midtarsal subluxation. Clin Orthop Relat Res. 1986; 209: 206-9. PMID: 3731597
- Tountas AA. Occult fracture-subluxation of the midtarsal joint. Clin Orthop Relat Res. 1989; 243: 195-9. PMID: 2721063
- Stutz JM, Karlin JM, Daly N. Fracture-dislocation of the talus in the pediatric patient. An unusual injury. J Am Podiatr Med Assoc. 1991; 81(9): 495-8. PMID: 1748966 DOI: 10.7547/87507315-81-9-495
- Skjodt K, Edal AL. Fracture-dislocation of Chopart’s junction. Ugeskr Laeger. 1995; 157(33): 4577-9. PMID: 7645104
- Kumagai S, Fitzgibbons TC, McMullen ST, et al. Chopart’s fracture dislocation: A case report and review of the literature. Nebr Med J. 1996; 81(4): 116-9. PMID: 8628450
- Miller CM, Winter WG, Bucknell AL, et al. Injuries to the midtarsal joint and lesser tarsal bones. J Am Acad Orthop Surg. 1998; 6(4): 249-58. PMID: 9682087 DOI: 10.5435/00124635-199807000-00006
- Richter M, Wippermann B, Thermann H, et al. Plantar impact causing midfoot fractures result in higher forces in Chopart’s joint than in the ankle joint. J Orthop Res. 2002; 20(2): 222-32. PMID: 11918301 DOI: 10.1016/S0736-0266(01)00096-1
- Rammelt S, Grass R, Schikore H, et al. Injuries of the Chopart joint. Unfallchirurg. 2002; 105(4): 371-83. PMID: 12066476 DOI: 10.1007/s00113-002-0440-5
- Sammarco VJ. The talonavicular and calcaneocuboid joints: Anatomy, biomechanics, and clinical management of the transverse tarsal joint. Foot Ankle Clin. 2004; 9(1): 127-45. PMID: 15062218 DOI: 10.1016/S1083-7515(03)00152-9
- Blackwood CB, Yuen TJ, Sangeorzan BJ, et al. The midtarsal joint locking mechanism. Foot Ankle Int 2005; 26(12): 1074-80. PMID: 16390642 DOI: 10.1177/107110070502601213
- Ip KY, Lui TH. Isolated dorsal midtarsal (Chopart) dislocation: A case report. J Orthop Surg (Hong Kong). 2006; 14(3): 357-9. PMID: 17200547 DOI: 10.1177/230949900601400327
- Strohm PC, Schwering L, Mehlhorn A, et al. Injuries of the midfoot in children. Unfallchirurg. 2006; 109(12): 1094-8. PMID: 17058063 DOI: 10.1007/s00113-006-1155-9
- Tweed JL, Campbell JA, Thompson RJ, et al. The function of the midtarsal joint: A review of the literature. Foot (Edinb). 2008; 18(2): 106-12. PMID: 20307420 DOI: 10.1016/j.foot.2008.01.002
- Swords MP, Schramski M, Switzer K, et al. Chopart fractures and dislocations. Foot Ankle Clin. 2008; 13(4): 679-93, viii. PMID: 19013402 DOI: 10.1016/j.fcl.2008.08.004
- Melao L, Canella C, Weber M, et al. Ligaments of the transverse tarsal joint complex: MRI anatomic correlation in cadavers. AJR Am J Roentgenol. 2009; 193(3): 662-71. PMID: 19696279 DOI: 10.2214/AJR.08.2084
- Puthezhath K, Veluthedath R, Kumaran CM, et al. Acute isolated dorsal midtarsal (Chopart’s) dislocation: A case report. J Foot Ankle Surg. 2009; 48(4): 462-5. PMID: 19577723 DOI: 10.1053/j.jfas.2009.01.016
- Klaue K. Treatment of Chopart fracture-dislocations. Eur J Trauma Emerg Surg. 2010; 36(3): 191-5. PMID: 26815861 DOI: 10.1007/s00068-010-1047-0
- van Dorp KB, de Vries MR, van der Elst M, et al. Chopart joint injury: A study of outcome and morbidity. J Foot Ankle Surg. 2010; 49(6): 541-5. PMID: 21035040 DOI: 10.1053/j.jfas.2010.08.005
- Schmitt JW, Werner CM, Ossendorf C, et al. Avulsion fracture of the dorsal talonavicular ligament: A subtle radiographic sign of possible Chopart joint dislocation. Foot Ankle Int. 2011; 32(7): 722-6. PMID: 21972769 DOI: 10.3113/FAI.2011.0722
- Lee SW, Kim DD, Buskanets A, et al. Midtarsal sprain misdiagnosed as ankle sprain: Role of ultrasonography in diagnosis. Am J Phys Med Rehabil. 2016; 95(3): e44-5. PMID: 26745218 DOI: 10.1097/PHM.0000000000000415
- Kutaish H, Stern R, Drittenbass L, et al. Injuries to the Chopart joint complex: A current review. Eur J Orthop Surg Traumatol. 2017; 27(4): 425-431. PMID: 28417204 DOI: 10.1007/s00590-017-1958-0
- De Dea M, Loizou CL, Allen GM, et al. Talonavicular ligament: Prevalence of injury in ankle sprains, histological analysis and hypothesis of its biomechanical function. Br J Radiol. 2017; 90(1071): 20160816. PMID: 27993094 DOI: 10.1259/bjr.20160816
- Walter WR, Hirschmann A, Tafur M, et al. Imaging of Chopart (midtarsal) joint complex: Normal anatomy and posttraumatic findings. AJR Am J Roentgenol 2018; 211(2): 416-25. PMID: 29927330 DOI: 10.2214/AJR.17.19310
- Hirschmann A, Walter WR, Alaia EF, et al. Acute fracture of the anterior process of calcaneus: Does it herald a more advanced injury to Chopart joint? AJR Am J Roentgenol. 2018; 210(5): 1123-30. PMID: 29570372 DOI: 10.2214/AJR.17.18678
- Walter WR, Hirschmann A, Alaia EF, et al. Normal anatomy and traumatic injury of the midtarsal (Chopart) joint complex: An imaging primer. Radiographics. 2019; 39(1): 136-52. PMID: 30500305 DOI: 10.1148/rg.2019180102
- Smith T, Ballard T, Ramanlal R, et al. Foot dislocation. 2020. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020. PMID: 32119500
- Main BJ, Jowett RL. Injuries of the midtarsal joint. J Bone Joint Surg Br. 1975; 57(1): 89-97. PMID: 234971
- Verhaar JA. Recurrent medial swivel dislocation of the foot. J Bone Joint Surg Br. 1990; 72(1): 154-5. PMID: 2298784
- Kennedy JG, Maher MM, Stephens MM. Fracture dislocation of the tarsal navicular bone: A case report and proposed mechanism of injury. Foot Ankle Surg. 1999; 5(3): 167-70. https://doi.org/10.1046/j.1460-9584.1999.00136.x
- Dhillon MS, Nagi ON. Total dislocations of the navicular: Are they ever isolated injuries? J Bone Joint Surg Br. 1999; 81(5): 881-5. PMID: 10530855 DOI: 10.1302/0301-620x.81b5.9873
- Tomcovcik L, Karolyi J, Kitka M. Swivel luxacia Chopartovho kibu. Acta Chir Orthop Traumatol Cech. 1999; 66(6): 362-6. PMID: 20478178
- Smith TF, Aguilar RG, Kurichh S. Dislocations. In: Banks AS, Downey MS, Martin DE, Miller SJ, eds. McGlamry’s comprehensive textbook of foot and ankle surgery. 3rd ed. Philadelphia: Lippincott Williams & Wilkins; 2001.
- Pillai A, Chakrabarti D, Hadidi M. Lateral swivel dislocation of the talo-navicular joint. Foot Ankle Surg. 2006; 12: 39-41. https://doi.org/10.1016/j.fas.2005.08.003
- Datt N, Rao AS, Rao DV. Medial swivel dislocation of the talonavicular joint. Indian J Orthop. 2009; 43(1): 87-9. PMID: 19753187 DOI: 10.4103/0019-5413.45329
- Williams DP, Hanoun A, Hakimi M, et al. Talonavicular dislocation with associated cuboid fracture following low-energy trauma. Foot Ankle Surg. 2009; 15(3): 155-7. PMID: 19635426 DOI: 10.1016/j.fas.2008.10.001
- Powell E, LaBella M. Swivel-type dislocation of the talonavicular joint: A case report. The Foot and Ankle Online Journal. 2011; 4(6): 3 doi: 10.3827/faoj.2011.0406.0003
- Inal S, Inal C. An unusual variety of simultaneous fracture dislocation pattern: Medial swivel dislocation of talonavicular joint with displaced fractures of the fourth and fifth metatarsals. J Foot Ankle Surg. 2013; 52(4): 501-4. PMID: 23664082 DOI: 10.1053/j.jfas.2013.04.006
- Bosman WM, Prakken FJ, Pijls BG, et al. Lateral talonavicular dislocation after low-energy trauma. BMJ Case Rep. 2013; 2013: bcr2013200692. PMID: 24001736 DOI: 10.1136/bcr-2013-200692
- Kapila R, Verka PS, Garg RS, et al. Lateral swivel dislocation of the hindfoot: A case report and literature review. J Foot Ankle Surg (Asia-Pacific). 2015; 2(1): 41-3. DOI: 10.5005/jp-journals-10040-1027
- Lasanianos NG, Kanakaris NK. Midtarsal bones: Chopart joint dislocations. In Lasanianos NG, Kanakaris NK, Giannoudis PV, eds. Trauma and orthopaedic classifications. London: Springer-Verlag; 2015.
- Jimenez I, Rodriguez-Alvarez JP, Navarro-Navarro R. Dorsal fracture-dislocation of the tarsal navicular. J Am Podiatr Med Assoc. 2017; 107(3): 226-230. PMID: 28650764 DOI: 10.7547/15-103
- Polat B, Aydın D, Polat AE, et al. Medial swivel dislocation of the talonavicular joint with associated cuboid fracture. J Am Podiatr Med Assoc. 2019; 109(4): 308-11. PMID: 31762306 DOI: 10.7547/17-191
- Kumar A, Gaba S, Digge VK, et al. Neglected medial swivel talonavicular dislocation treated with arthrodesis: A case report and literature review. J Clin Orthop Trauma. 2020; 11(3): 474-8. PMID: 32405213 DOI: 10.1016/j.jcot.2018.12.011
- Magnusson EA, Hreha J, Taitsman L. Other midfoot dislocations. In Adams MR, Benirschke SK, eds. Fractures and dislocations of the talus and calcaneus. Springer Nature Switzerland AG; 2020.
- Ross PM, Mitchell DC. Dislocation of the talonavicular joint: Case report. J Trauma. 1976; 16(5): 397-401. PMID: 1271504 DOI: 10.1097/00005373-197605000-00014
- Meister K, Demos HA. Fracture dislocation of the tarsal navicular with medial column disruption of the foot. J Foot Ankle Surg. 1994; 33(2): 135-7. PMID: 8019533
- Samoladas E, Fotiades H, Christoforides J, et al. Talonavicular dislocation and nondisplaced fracture of the navicular. Arch Orthop Trauma Surg. 2005; 125(1): 59-61. PMID: 15592933 DOI: 10.1007/s00402-004-0769-z
- Khazim R, Salo PT. Talar neck fracture with talar head dislocation and intact ankle and subtalar joints: A case report. Foot Ankle Int. 1995; 16(1): 44-8. PMID: 7697154 DOI: 10.1177/107110079501600110
- Hafez MA, Bawarish MA, Guvvala R. Closed talar body fracture with talonavicular dislocation; a case report. Foot Ankle Int. 2000; 21(7): 599-601. PMID: 10919629 DOI: 10.1177/107110070002100714
- Ricci WM, Bellabarba C, Sanders R. Transcalcaneal talonavicular dislocation. J Bone Joint Surg Am. 2002; 84(4): 557-61. PMID: 11940615 DOI: 10.2106/00004623-200204000-00008
- Newton Ede MP, Miller C, Malik MH, et al. An unusual case of talonavicular dislocation with associated ipsilateral foot fractures. J R Army Med Corps. 2006; 152(2): 102-3. PMID: 17175774 DOI: 10.1136/jramc-152-02-07
- Galanakos SP, Papathanasiou V, Sofianos IP. Transcalcaneal talonavicular dislocation associated with an open comminuted calcaneal fracture: A case report. Clin Podiatr Med Surg. 2011; 28(4): 763-7. PMID: 21944406 DOI: 10.1016/j.cpm.2011.07.002
- Schmid T, Krause F, Gebel P, et al. Operative treatment of acute fractures of the tarsal navicular body: Midterm results with a new classification. Foot Ankle Int. 2016; 37(5): 501-7. PMID: 26704174 DOI: 10.1177/1071100715624208
